Patient Information

Reduce of stop the flow of your period in less that two and a half minutes
Thermablate is a minimally invasive one time treatment option for pre menopausal women suffering from heavy menstrual bleeding due to begin causes who have completed childbearing

Do you feel like your life revolves around your periods?
Heavy menstrual bleeding affects 1 in 5 women and can have a negative impact on their life. Heavy menstrual bleeding, known medically as menorrhagia, affects women physically and mentally. It can affect your mood, energy, work, social life and your general well-being.
Approximately one half of all cases of heavy menstrual bleeding have no obvious cause. In other cases, the possibility of uterine abnormalities or hormonal imbalances may exist. Other physical problems may also cause menorrhagia and might include uterine fibroids or polyps, infection, cancer, or a bleeding disorder.
You might have menorrhagia if you have:
- A heavy menstrual flow that keeps you from carrying out your daily routine
- Menstrual periods that include large blood clots
- Menstrual periods lasting longer than one week
- Symptoms resembling anaemia or feelings of fatigue
How do we treat menorrhagia?
Non-surgical options
Drug therapy (birth control pills or other types of hormones) or intrauterine devices are typically the first treatment option for women who wish to maintain fertility. It is not always effective in controlling excessive bleeding and some women may experience side effects.
Surgical options
Dilatation and curettage: a procedure that removes endometrium and may provide temporary relief of heavy periods lasting only a few cycles. This may be a treatment option for women who want more children.
Hysterectomy: is the removal of the uterus and is a major surgical procedure. It is performed in a hospital under general anaesthesia. It may require hospitalisation and a recovery period of up to six weeks.
Hysteroscopic endometrial ablation: eliminates the lining of the uterus with an electrosurgical tool or laser. This requires general anaesthesia and is also associated with increased surgical risks. This is not appropriate for women wanting to maintain fertility. Risks may include: uterine perforation, bleeding, infection and heart/lung failure due to fluids required in the procedure.
New minimally invasive endometrial ablation methods: there are a variety of new generation endometrial ablation devices that use different methods to destroy the lining of the uterus. These include heated fluid systems and radiofrequency energy systems. Endometrial ablation allows for fast recovery with return to normal activities within a few days. Risks are reduced compared to other surgical methods and may include uterine perforation, bleeding, infection, cramping, vaginal discharge, injury to other organs, or burns.
All methods carry risks, although they are reduced in less invasive methods. The method of treatment used will be dependent upon the patient’s individual circumstances and should be discussed with their doctor.
What is Thermablate?
Thermablate is a clinically proven, gentle two and a half minute treatment that can significantly reduce or stop the flow of your menstrual period.
Thermablate is:
A safe, minimally invasive treatment for menorrhagia
An alternative to hysterectomy or other surgical treatment
A well tolerated outpatient treatment requiring no hospital stay
Effective: in studies comparing various treatment options, 95% of women reported the greatest improvement in menorrhagia with Thermablate with 85% of them experiencing a dramatic or complete reduction in bleeding
For whom is Thermablate the right treatment?
The Thermablate system is used in premenopausal women with menorrhagia due to benign causes for whom child bearing is complete. A physician will perform some preliminary tests which may include blood work, hysteroscopy, biopsy, and/or a Pap smear to determine the cause of the patient’s bleeding.
Endometrial ablation, by any method, is not an option for those wishing to maintain fertility,
How does Thermablate work?
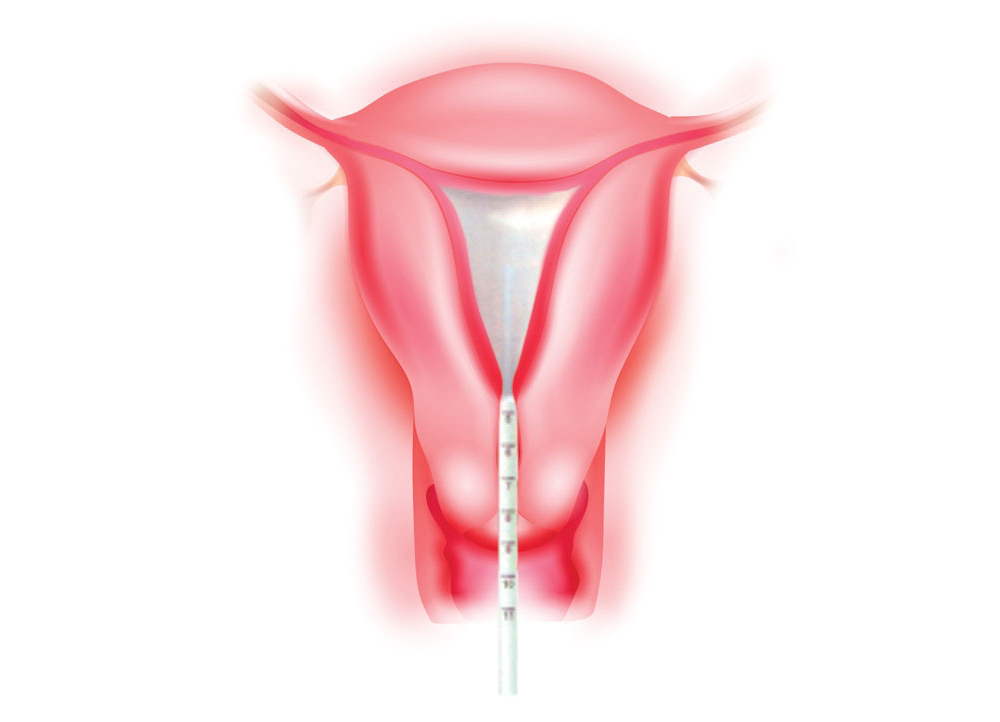
The treatment can be done in an outpatient clinic or the operating room depending on whether you want to be awake or fully asleep.The doctor will gently insert a soft, flexible silicone balloon attached to a thin catheter into your uterus. The balloon is inflated with heated glycerin solution and expands to fit the size and shape of the uterus. The patient and physician will decide what type of pain medication is best suited to relieve cramping and discomfort.
After the treatment
The physician may prescribe medication if patients experience some discomfort such as cramping. Other symptoms you may experience are nausea and vomiting. Patients will normally be allowed to go home within a few hours. Patients can usually resume work and family commitments the following day. It is typically recommended that patients refrain from sexual activity and the use of tampons for one week after the treatment in order to reduce the risk of infection.
Ablation and Pregnancy
A Thermablate treatment does not prevent patients from becoming pregnant. Pregnancy after any type of ablation treatment can result in serious health complications. Patients should discuss contraception options with their physician.
Choose Simplicity
The vast majority of women experience positive changes in their life after a Thermablate procedure. These may include:
- Freedom to live a normal life
- Financial benefits
- Better health
- Increased energy
Women worldwide choose to have a Thermablate treatment to improve every aspect of their lives.
To learn more about Thermablate EAS, please visit our manufacturer partner website here
CONTACT US TODAY


