
Thermablate EAS is a minimally invasive one time treatment option for pre menopausal women suffering from heavy menstrual bleeding due to begin causes who have completed childbearing

About Thermablate EAS
The Thermablate Endometrial Ablation System is a clinically proven, gentle, two minute treatment that can significantly reduce or stop heavy menstrual periods for women who have completed childbearing. Thermablate EAS is a one-time, non-hormonal treatment that reduces the need for major surgical intervention such as hysterectomy.
The Thermablate EAS is made up of a Treatment Control Unit and disposable cartridge, often referred to as a balloon catheter.
The Treatment Control Unit is:
- Fully automated
- Simple to set up
- Compact, lightweight

How does Thermablate EAS work?
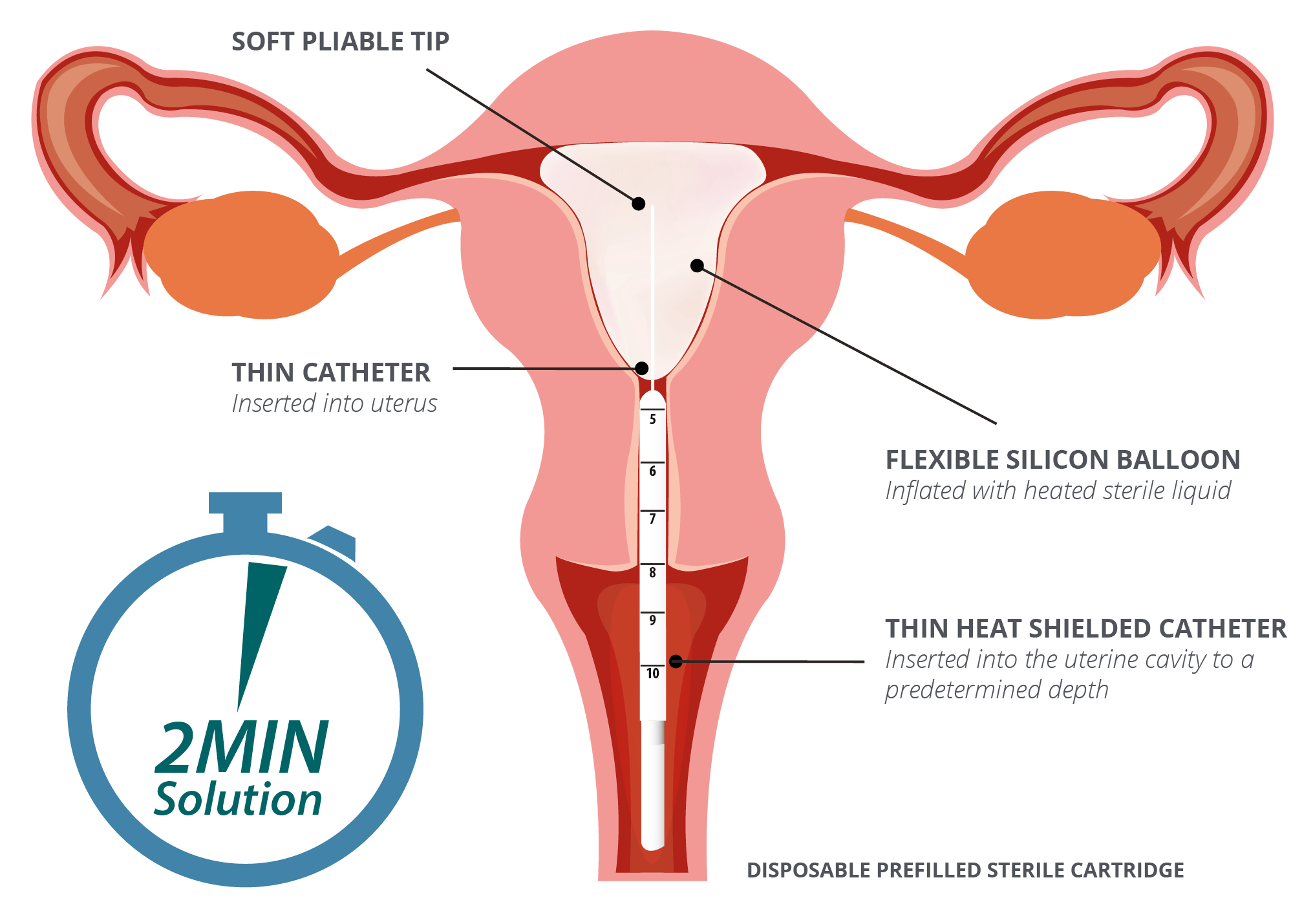
- A heat shielded catheter is inserted into the uterine cavity
- At the tip of this catheter, there is a soft tipped silicone balloon
- A heated sterile liquid flows through the catheter and into the balloon
- The balloon conforms to the shape of the cavity, gently touching the lining of the uterus
- The balloon inflates and deflates 3 times during the 2 minute procedure
- Through this emission of heat, the endometrium is destroyed
Patient Selection
Proper patient selection is very important to consider. Not all women can undergo a Thermablate treatment. Patients should always be evaluated thoroughly prior to treatment to rule out any underlying causes of their excessive uterine bleeding.

Endometrial ablation, by any method, is not an option for those wishing to maintain fertility.
CONTACT US TODAY

